Common Foot and Ankle Disorders
Heel Pain
Description
 The most common form of heel pain, is pain on the bottom of the heel, called plantar heel pain. It tends to occur for no apparent reason and is usually worse when first placing weight on the foot in the morning or after a period of time sitting. The pain can be a sharp, searing pain or present as a tearing feeling in the bottom of the heel.
The most common form of heel pain, is pain on the bottom of the heel, called plantar heel pain. It tends to occur for no apparent reason and is usually worse when first placing weight on the foot in the morning or after a period of time sitting. The pain can be a sharp, searing pain or present as a tearing feeling in the bottom of the heel.
To understand the cause of the pain one must understand the anatomy of the foot and some basic mechanics in the function of the foot. A thick ligament, called the plantar fascia, is attached into the bottom of the heel and fans out into the ball of the foot, attaching into the base of the toes. The plantar fascia is made of dense, fibrous connective tissue that will stretch very little. It acts something like a shock absorber and as one of the supporters of the arch of the foot. As the foot impacts the ground, the foot flattens out putting the plantar fascia under tension. As the plantar fascia comes under tension it stretches slightly. Anything that causes the foot to flatten excessively will cause the plantar fascia to stretch greater than it is accustomed to doing.
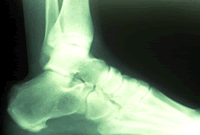 One consequence of this is the development of 1) small tears in the ligament just in front of where it originates on the heel bone, and 2) small tears in the periosteum - "bone skin" - causing the growth of "new bone" and the formation of a heel spur. The pain experienced in the bottom of the heel is rarely if ever from walking on the spur, rather the pain is from the inflammation and irritation to nerves within the plantar fascia and the periosteum, the point where the plantar fascia attaches on the bottom of the heel bone. When the foot rests, the swelling due to inflammation increases. The inflammation is actually the body's attempt to heal itself. But, this inflammation and swelling also puts excessive pressure on nerves, which then only needs a little bit of extra pressure, say from standing on it, to them become extremely painful. People often say that if they walk on the painful heel for 15 to 30 minutes the pain will go away; This is because walking pushes out the swelling that built-up when the foot was resting.
One consequence of this is the development of 1) small tears in the ligament just in front of where it originates on the heel bone, and 2) small tears in the periosteum - "bone skin" - causing the growth of "new bone" and the formation of a heel spur. The pain experienced in the bottom of the heel is rarely if ever from walking on the spur, rather the pain is from the inflammation and irritation to nerves within the plantar fascia and the periosteum, the point where the plantar fascia attaches on the bottom of the heel bone. When the foot rests, the swelling due to inflammation increases. The inflammation is actually the body's attempt to heal itself. But, this inflammation and swelling also puts excessive pressure on nerves, which then only needs a little bit of extra pressure, say from standing on it, to them become extremely painful. People often say that if they walk on the painful heel for 15 to 30 minutes the pain will go away; This is because walking pushes out the swelling that built-up when the foot was resting.
There are some less common causes of bottom heel pain such as bone fractures, infection, arthritis, tumors, etc., but they account for less than 5% of plantar heel pain. (Note: Heel pain on the back of the heel has causes similar in origin to bottom heel pain - which is excessive tension where the Achilles Tendon attaches resulting in the growth of new bone, which in turn cuts up and into the Achilles Tendon. In this instance, reducing tension will help alleviate the pain, though in a substantial percentage of cases surgery is required to remove the sharp bone and reattach the Achilles Tendon. BUT, this pain must never be treated with injections of cortisone.)
There are several factors that cause the foot to flatten and excessively stretch the plantar fascia. The primary factor is the structure of a joint complex below the ankle joint, called the subtalar joint. The movement of this joint complex causes the arch of the foot to flatten and to heighten. Flattening of the arch of the foot is termed pronation and heightening of the arch is called supination. If there is excessive pronation of the foot during walking and standing, the plantar fascia is strained.
Another factor that contributes to the flattening of the arch of the foot is tightness of the calf muscles and or the Achilles Tendon itself. The calf muscle attaches into the foot by the Achilles Tendon into the back of the heel. When the calf muscle is tight it limits the movement of the ankle joint. When ankle joint motion is limited by the tightness of the calf muscle it forces the subtalar joint to pronate excessively causing the foot to flatten excessively. This excessive subtalar joint pronation can cause several different problems to occur in the foot, which in the case of heel pain results in excessive tension and stretching of the plantar fascia.
Diagnosis
The diagnosis of heel pain and heel spurs is made by a through history of the course of the condition and by physical exam together with weight bearing x-rays. Often an MRI is needed as well. Blood testing is sometimes ordered in order to rule out infection, gout, and or arthritis.
Treatment
Treatment of heel pain generally occurs in stages. At the earliest sign of heel pain, calf and Achilles Tendon stretches should be started, together with the wearing of work and athletic shoes with at least a difference of 1 inch between the front and back of the shoe. (This regimen should continue at all times when on the feet, especially at home!) Additionally, taking an oral anti-inflammatory medication such as "Advil" can be helpful. And, the first course of treatment would include an injection of local anesthetic mixed with a small amount of corticosteroid - the purpose of which is to stop the painful inflammation - breaking the pain cycle and allowing a return to normal more pain-free walking and standing. Two or maybe three total injections can be given, but one should wait at least one month between each injection. The use of a night splint, which holds the foot at 90 degrees, stretching the calf muscles and the Achilles tendon, is often used.
If these approaches fail, and if all attempts are made to insure that there are no reasons for the pain other than mechanics and damage to the plantar fascia, the next treatment options include the newest "shock wave" therapy and then finally the surgical approach called the "endoscopic plantar fasciotomy".
Shock wave therapy is not well understood. This technology uses the same kind of device that is used to break-up kidney stones - "injecting" powerful sound waves deep into the tissues. The waves are focused onto the area of pain. The theory is that the many months or years of inflammation have caused the painful tissues to become scarred and thickened, which has entrapped nerves. The shock waves supposedly break-up the scar tissue, stretch the scar tissue alleviating some of the tension, and then promote the normal healing of the damaged thickened areas of the plantar fascia. Tens of thousands of patients have been treated by this method, the majority with good results. The best thing about this method is that it can do no harm, and if it works - surgery has been avoided.
Endoscopic plantar fasciotomy is the final treatment option available when "all else fails". 5% of patients will not respond to non-surgical treatment. The endoscopic method is patterned after a technique first used to release the carpal tunnel (a hand condition), a technique that avoids the use a large incision. In an operating room, under local anesthesia (or general anesthesia), a small tube with a "window" on one side enters the heel through a very small incision on the inside, exiting through a very small incision on the outside. Using a very small camera to guide the surgeon, a little knife cuts the tight plantar fascia, lengthening it, taking tension away. Patients walk on the foot immediately thereafter, returning to normal shoes within several days, and normal activities within several weeks. Because most bottom heel pain can be treated without surgery, and because this technique can sometimes cause painful scaring and structural changes to the foot, it is always the option of last resort.
